Definisjon
Sweets syndrom er en betennelsesaktig sykdom med brå start. Feber-anfall og angep på hud, øyne, muskler, ledd og organer er typisk. Sweets syndrom er beslektet med andre neutrofile dermatoser som pyoderma gangrenosum (hud), neutrofil hidradenitt (svettekjertler), og Behçets sykdom (sår i munn og underlig). Sweets syndrom kan utløses av kreftsykdom, men også av medikamenter eller uten kjent bakenforliggende årsak (referanse: Vashisht P, 2021). Tilstadnen ble beskrevet i 1964 av RD Sweet (referanse: Sweet RD, 1964).
Forekomst
Sweets syndrom er sjelden, men vanligst blant middelaldrende kvinner, 30-60 år. Kvinner: menn: 4:1. Den er også beskrevet hos barn (referanse: Vashisht P, 2021).
Symptomer
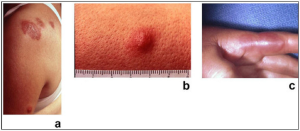
- Brå start med feber og utslett er typisk.
- Utslettet kommer plutselig og består av ømme knuter (papler) eller harde flekker (plakk) som går i dybden.
- Noen får også såre øyne og munnsår, ledd- og hodesmerter.
- Sjeldnere er symptomer fra indre organer
Disponerende tilstander
Infeksjon i luftveier, vaksinasjon, kronisk tarmsykdom (IBD (ulcerøs kolitt eller Crohn’s sykdom)), leddgikt/Revmatoid artritt, blodsykdommer, inklusiv leukemi: Oftest akutt myelogen leukemi. Annen kreftsykdom påvises oftest i tarm, urinveier eller i bryster. Også svangerskap kan disponere.
Undersøkelser
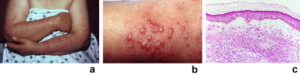
Sykehistorien kartlegger disponerende tilstander og aktuelle symptomer (se ovenfor). Vekttap og allmennsymptomer etterspørres.
Klinisk undersøkes hud-manifestasjonene som består av blemmer (pustler, bulla), sår (ulcerasjoner) som kan avbleke i senter. Kan iblant ligne pyoderma gangrenosum. Lokalisasjonen er oftest på oversiden av hender, men også ansikt, hals, bryst, rygg og ben kan angripes. Utselttet øker i størrelse og varer over flere uker. I likhet med Behcets syndrom kan patergi-test slå ut.
Feber er til stede hos 80-90%, særlig der medikamenter er utløsende. Utmattelse og hodepine er andre allmennsymptomer. Revmatisk ser leddsmerter eller leddbetennelser (artritt) hos 20-60%. Muskelsmerter forekommer også.
Øyet kan angripes i form av overfladisk betennelse (konjunktivitt), sjeldnere dypere betennelse som episkleritt, skleritt, keratitt og uveitt (referanse: Gottlieb CC, 2008).
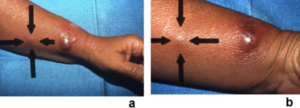
Blodprøver. Rutineprøver kan omfatte CRP, SR, hgb, hvite blodlegemer med differensialtelling, blodplater, elektrolytter, lever-, nyre-, og thyreoidea-funksjonsprøver, CK, proteinelektroforese og urin-stiks. Blodsenkningsreaksjon (SR) og CRP er forhøyet (systemisk inflammasjon). Økt antall hvite blodlegemer (neutrofil leukocytose). Svangerskapstest ved mulig graviditet.
Inge spesielle revma-tester/antistoff forventes å slå ut, men anti-CCP, ANCA, ANA, anti-DNA og antifosfolipid antistoff kan tas for å utelukke lignende tilstander (se nedenfor).
Bildediagnostikk. Med tanke på bakenforliggende kreft vurderes indikasjon for CT lunger, mage-område (abdomen) og bekken, samt mammografi, ev. PET/CT.
Koloskopi ved behov for å utelukke koloncancer.
Vevsprøve (biopsi). Hudbiopsi: viser i dybden mange neutrofile granulocytter som er en type hvite blodlegemer (neutrofil dermatose) og destruerte celler (leukocytoklastisk), samt ødematøse endotel celler i blodårevegger (vaskulitt).
Diagnosen
Oftest stilles diaagnosen på bakgrunn av sykehiustorie, klinisk undersøkelse og ikke minst vevspørven ved fravær av lignende tilstander. Det er også utviklet diagnostiske kriterier (se ev Grans Kompendium i Revmatologi).
Sykdomsforløp
En eller flere røde og ømme knuter i eller under huden som øker i størrelse og varer i flere uker. Hudforandringene kan også ha blemmer (pustler), sår (ulcerasjoner) og kan avbleke i senter. Kan iblant ligne pyoderma gangrenosum
lignende sykdommer / differensialdiagnoser
- Allergisk kontaktdermatitt
- Behcets sykdom
- Dermatomyositt
- DRESS syndrom og andre hudreaksjoner på medikamenter
- Infeksjon / sepsis / erysipelas
- Endokarditt (infeksjon)
- Herpes simpleks
- Herpes zoster
- Leukocytoklastisk vaskulitt
- Leukemia cutis
- Lymfom
- Mycobakterium marinum (hud, ledd, feber)
- PAN (Polyarteritis nodosum)
- Pannikulitt
- Pyoderma gangrenosum
- Roseacea
- Serumsyke/hypersensitivitetssyndrom
- Soppinfeksjon, Systemisk mykose
- Systemisk lupus (SLE)
- Tuberkulose (Tbc)
- VEXAS syndrom
Behandling
Steroider (Prednisolon) blir brukt først. Lokale kortikosteroid-injeksjoner kan også vurderes. Hvis ikke tilstrekkelig effekt og residiverende lesjoner brukes kaliumjodid eller Kolkisin. Alternativer er ciclosporin, metotreksat IVIG, rituksimab, eller vedolizumab (Entyvio) (referanse: Vashisht P, 2021). NSAIDs kan lindre symptomer.
Prognose
Hud-symptomene går spontant tilbake etter 4-8 uker, men kan komme tilbake. Omtrent 15-20% utvikler kreftsykdom.

